In this article:
Components of Meig's syndrome
Epidemiology
Clinical presentation
Differential diagnosis
Investigations
Associated diseases
Management
Prognosis
Components of Meig's syndrome
Epidemiology
Clinical presentation
Differential diagnosis
Investigations
Associated diseases
Management
Prognosis
Components of Meig's syndrome
Dr Joe Vincent Meigs proposed limiting the diagnosis of Meigs' syndrome to benign and solid ovarian tumours with ascites and pleural effusion, and with the condition that removal of the tumour cures the patient without recurrence. To conform to the diagnosis of true Meigs' syndrome the ovarian tumour may be a fibroma, thecoma, cystadenoma, or granulosa cell tumour. If the tumour is resected, the fluid resolves. |
| Schematic drawing of female reproductive organs, frontal view. CDC, Mysid / Public domain |
- A benign ovarian tumour (a fibroma, or fibroma-like tumour).
- Ascites.
- Pleural effusion.
Epidemiology
Meigs' syndrome is a rare condition. Fibromas account for around 3% of all ovarian tumours in women, and Meigs' syndrome for 1-2% of those. Meig's syndrome tends to occur most often in postmenopausal women, with an average age of presentation of around 50 years.Clinical presentation
Most of the clinical features of the Meig's syndrome are related to ascites and pleural effusion; however before the menopause there may be menstrual symptoms too. Common symptoms which may trouble a person include:- Fatigue.
- Breathlessness (initially on exertion).
- Pelvic pain or bloating.
- Constipation.
- Swollen abdomen with associated weight gain or weight loss.
- Non-productive cough.
- Amenorrhoea (no menses) or irregular menstruation.
Examination findings
If the doctor examines a person with Meig's syndrome, they may discover the following:- Reduction in lung capacity which may produce fast breathing (tachypnoea) and fast rate of heart beat (tachycardia).
- Examination of the chest will revealing dullness to percussion over the pleural effusion. There will be decreased breath sounds and decreased tactile vocal fremitus (intensity of vibrations of the chest wall created with certain spoken words in a constant tone and voice).
- The effusion tends to be right-sided but can be bilateral. There appears to be no adequate explanation for this unilaterality. A large right-sided effusion will displace the mediastinum to the left with deviation of the trachea to the left and displacement of the apex beat.
- Abdominal examination may reveal a tumour arising from the pelvis but this may be obscured by ascites. The features of ascites include a fullness of the flanks and shifting dullness.
- Pelvic examination may reveal an ovarian mass.
Differential diagnosis
The main differential diagnosis is a malignant ovarian tumour because:- they are much more common than Meigs' syndrome and tend to produce profuse ascites with a high protein content.
- pleural effusion is a less common presentation unless due to pulmonary metastases.
- Other cancers, particularly colon.
- Metastatic breast cancer.
- Tuberculosis.
- Nephrotic syndrome.
- Congestive heart failure.
- Cirrhosis.
Investigations
- Your urine will be checked for presence of protein.
- You would get routine blood tests done including full blood count (FBC), urea and electrolytes (U&E), liver function tests (LFTs), including plasma proteins.
- Cancer antigen 125 (CA 125) is often elevated both in serum and in pleural and peritoneal fluid. So you should get checked for this.
However, CA 125 is not reliable and cases have been described with very high CA 125 and with normal levels. It can also be normal in ovarian malignancy. - Chest x-ray (AP and lateral) will show the degree of pleural effusion.
- Abdominal ultrasound will demonstrate the ascites and should outline the ovarian tumour too.
- Imaging also includes CT of the chest, abdomen and pelvis, and MRI of the pelvis.
- Paracentesis and aspiration of pleural fluid:
These procedures also help to relieve symptoms. Fluid should be sent for cytology. This is very important in distinguishing malignant ascites from Meigs' syndrome.
The fluid tends to have the features of an exudate, although some studies describe it as a transudate. In ovarian carcinoma the protein content is usually high.
Your pleural and ascitic fluid should also be examined for protein, glucose, amylase, cell count, organisms and AAFB if indicated. - If your doctor suspects congestive heart failure, an ECG will be required. Echocardiogram is indicated only if the ECG is abnormal.
Associated diseases
Pseudo-Meigs' syndrome is characterised by pleural effusion, ascites and benign ovarian tumours other than fibromas as described by Meigs. The tumours may include those of the Fallopian tube, uterus, round ligament, mature teratomas, struma ovarii or ovarian leiomyomas, as well as those originating in the colon, breast and stomach.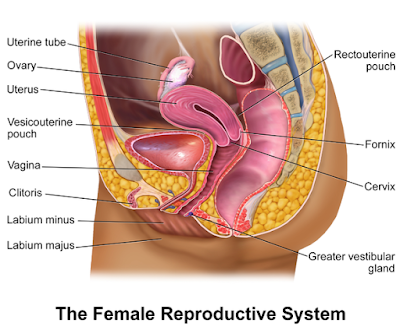 |
| A sectional view. Credit: BruceBlaus / CC BY |
Atypical Meigs' syndrome consists of a benign pelvic mass with a right-sided pleural effusion but no ascites present. This is rare. The pleural effusion resolves after resection of the tumour.
Management
The essential management is surgical removal of the tumour. Before operation, aspiration of pleural effusion and ascites may be required to improve pulmonary function.The operation includes full laparotomy to exclude other causes of malignancy, including bowel:
- In women of reproductive age a unilateral salpingo-oophorectomy is usually performed.
- In girls who are before the menarche, wedge resection may be preferred if feasible.
- After the menopause an operation of total abdominal hysterectomy with bilateral salpingo-oophorectomy is usual.
Prognosis
Within weeks to months of operation the ascites and pleural effusion resolve and the CA 125 returns to normal. Postoperative resolution of the fluid is part of the definition of the disease. As it is a benign tumour the prognosis is excellent. If there is functioning ovarian tissue, fertility should be preserved.Reference(s)
1). Whonamedit.com: Joe Vincent Meigs. Available online: http://www.whonamedit.com/doctor.cfm/2082.html
2). Riker D, Goba D: Ovarian mass, pleural effusion, and ascites: revisiting Meigs syndrome.. J Bronchology Interv Pulmonol. 2013 Jan20(1):48-51. doi: 10.1097/LBR.0b013e31827ccb35. Available online here.
3). Yamamoto A, Miyasaka Y, Furuya K, et al: Pseudo-Meigs' syndrome due to ovarian metastases from colon cancer: a case report and review of the literature.. Surg Case Rep. 2016 Dec2(1):112. Epub 2016 Oct 12. Available online here.
4). Cha MY, Roh HJ, You SK, et al: Meigs' syndrome with elevated serum CA 125 level in a case of ovarian fibrothecoma. Eur J Gynaecol Oncol. 201435(6):734-7. Available online here.
5). Krenke R, Maskey-Warzechowska M, Korczynski P, et al: Pleural Effusion in Meigs' Syndrome-Transudate or Exudate?: Systematic Review of the Literature Medicine (Baltimore). 2015 Dec94(49):e2114. doi: 10.1097/MD.0000000000002114. Available online here.

No comments:
Post a Comment
Got something to say? We appreciate your comments: